Vaccines Covered by Medicare
Medicare Part B covers the shots, vaccines and immunizations that most people need, including a yearly flu shot. These preventive services are provided at no cost to you. Medicare Part D prescription drug plans can cover some costs of other common shots.
- Written by Terry Turner
Terry Turner
Senior Financial Writer and Financial Wellness Facilitator
Terry Turner has more than 35 years of journalism experience, including covering benefits, spending and congressional action on federal programs such as Social Security and Medicare. He is a Certified Financial Wellness Facilitator through the National Wellness Institute and the Foundation for Financial Wellness and a member of the Association for Financial Counseling & Planning Education (AFCPE®).
Read More- Edited By
Lamia Chowdhury
Lamia Chowdhury
Financial Editor
Lamia Chowdhury is a financial content editor for RetireGuide and has over three years of marketing experience in the finance industry. She has written copy for both digital and print pieces ranging from blogs, radio scripts and search ads to billboards, brochures, mailers and more.
Read More- Reviewed By
Christian Worstell
Christian Worstell
Medicare Expert
Christian Worstell is a licensed health insurance agent and an established writer in the sector, with articles featured in Forbes, MarketWatch, WebMD and more. His work has positively impacted beneficiaries nationwide and empowers them to make strong health care decisions.
Read More- Published: July 9, 2020
- Updated: October 13, 2023
- 5 min read time
- This page features 5 Cited Research Articles
- Edited By
- Medicare Part B covers several important annual vaccines such as the flu shot and Hepatitis B.
- Medicare Part D covers different vaccines such as shingles and Tdap, some with co-pay, others entirely.
- Your local pharmacy will often be able to provide vaccinations if they accept Medicare.
Are Vaccinations Covered by Medicare?
Medicare covers some, not all, of the vaccines recommended by the Centers for Disease Control’s Advisory Committee on Immunization Practices (ACIP). While Medicare Part B (part of Original Medicare) covers some vaccines, others are covered under Medicare Part D. Medicare Part D is not included in Original Medicare.
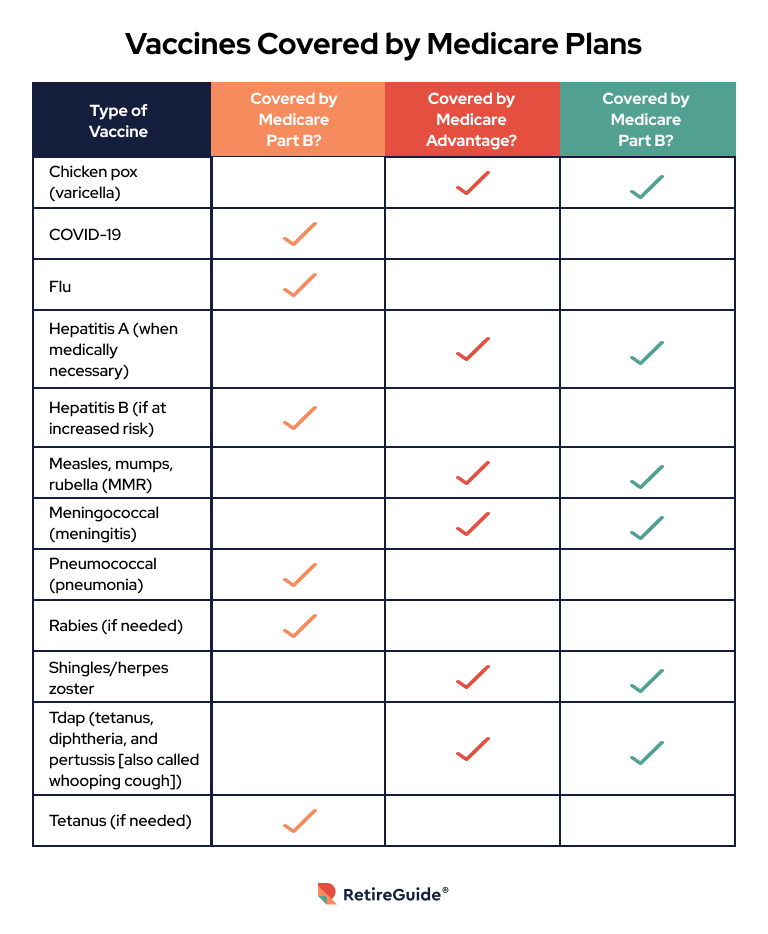
In 2023, additional vaccines will be fully covered by some Medicare plans.
“Many vaccines are free with Medicare, so it’s wise to take advantage of the benefit. And a free vaccine now can prevent a costly disease in the future. Medicare beneficiaries are encouraged to speak to their doctor about the vaccines that are available to them.”
Vaccines Covered by Medicare Part B
Medicare Part B covers several vaccines that play a vital role in preventing disease and maintaining health. These vaccines and other preventive services are available to you at no cost.
Which Vaccines Does Medicare Part B Cover?
- Flu Shot
- Medicare Part B fully covers one flu shot each flu season. The shot is either a regular strength dose or the high strength dose for extra immunity.
- Pneumococcal Vaccinations
- Medicare covers two different pneumococcal shots which protect you from different strains of pneumonia-causing bacteria. Many people need only one shot; however, a second, different shot is covered 11 months after the first shot.
- Hepatitis B
- Medicare fully covers Hepatitis B shots for people at medium or high risk for the disease. Check with your doctor to see if you qualify.
- COVID-19 Vaccine
- Medicare also covers COVID-19 vaccines, including the recently updated version targeting new strains and the Omicron variants.
Other vaccines, like a tetanus or rabies shot, are covered by Medicare Part B if they are related to a doctor’s treatment of an injury or illness.
Certain vaccines that are not under Medicare Part B coverage can be paid for through your Medicare Part D plan.
Vaccinations Covered by Medicare Part D
Medicare Part D, the prescription drug plan, pays for commercially available vaccines not covered by Medicare Part B.
According to the Centers for Medicare and Medicaid Services, a medical professional must deem the shot reasonable and necessary to prevent illness, and your co-pays will vary according to your particular plan.
Part D plans use a formulary, a list of drugs and shots, to indicate exactly which measures are covered by each plan. Formularies are designed to meet the needs of most members. However, your plan may still cover certain new vaccines, even if they do not appear in the formulary.
Part D plans often have special rules for vaccines, such as needing prior authorization from your doctor or quantity limits. Contact your plan provider for your specific coverage details.
Medicare Advantage (Part C) plans that include prescription drug coverage usually also cover all commercially available vaccinations.
Costs for Part D-Covered Vaccinations
Starting in Jan. 2023, immunizations recommended by ACIP, including the shingles and Tdap vaccines, will be covered by Medicare Part D with no deductible and no copay, as part of the Inflation Reduction Act.
Otherwise, how much you pay for Part D shots can vary depending on your plan and where you get vaccinated.
You can receive vaccinations at an in-network pharmacy or your doctor’s office. Your doctor can also coordinate with your pharmacy to directly bill your Part D plan for the vaccination, so you will only owe your plan’s coinsurance or copay.
Make sure to check your plan’s coverage rules to find the most affordable place to get vaccinated
How To Get Vaccinated
Not all medical providers can administer every vaccine. Your state or local health department should offer a list of providers near you if you don’t have a primary care physician or nearby pharmacy.
Doctor’s Office vs. Pharmacy
Your local pharmacy will often be able to provide vaccinations if they accept Medicare. Your primary health physician or clinic is another excellent choice.
Some vaccines require a doctor’s prescription; others will be available without one.
Typical Vaccine Schedule for Older Adults
The goal of vaccination is prevention. As you age, childhood vaccines lose their efficacy and new health concerns arise. Even if you are healthy, it is important to keep up with medically recommended vaccinations. This could save you time and money in the future.
The Centers for Disease Control and Prevention (CDC) has an updated list of recommended vaccines for adults. In addition to COVID-19 and annual flu shots, the CDC encourages adults over 50 to get shingles and pneumococcal vaccines, as well as a Tdap booster. They also recommend the Hepatitis B vaccine for adults aged 60 and up, especially if you have risk factors for the disease.
Frequently Asked Questions About Medicare Coverage for Vaccines
Editor Samantha Connell contributed to this article
5 Cited Research Articles
- Centers for Disease Control and Prevention. (2022, November 23). Advisory Committee on Immunization Practices. Retrieved from https://www.cdc.gov/vaccines/acip/index.html
- Centers for Medicare & Medicaid Services. (2022, October 5). Reduced Drug Prices, Enhanced Medicare Benefits Under the Inflation Reduction Act Frequently Asked Questions (FAQs). Retrieved from https://www.cms.gov/files/document/10522-external-faqs-about-inflation-reduction-act.pdf
- Centers for Disease Control and Prevention. (2022, March 30). What Vaccines are Recommended for You. Retrieved from https://www.cdc.gov/vaccines/adults/rec-vac/index.html
- Centers for Disease Control and Prevention. (2019, August 1). Get Vaccinated Before You Travel. Retrieved from https://www.cdc.gov/vaccines/parents/travel-vaccines.html
- Medicare.gov. (n.d.). Coronavirus Disease 2019 (COVID-19). Vaccine. Retrieved from http://www.medicare.gov/coverage/coronavirus-disease-2019-covid-19-vaccine
Calling this number connects you to one of our trusted partners.
If you're interested in help navigating your options, a representative will provide you with a free, no-obligation consultation.
Our partners are committed to excellent customer service. They can match you with a qualified professional for your unique objectives.
We/Our Partners do not offer every plan available in your area. Any information provided is limited to those plans offered in your area. Please contact Medicare.gov or 1-800-MEDICARE to get information on all of your options.
888-694-0290Your web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you need help pricing and building your medicare plan, call us at 844-572-0696


