When Your Golden Years Feel Blue: Recognizing and Battling Depression in the Elderly
There may be no life transition as jarring as retirement. While we often think of leaving the workforce behind as a lifetime achievement and something to plan toward, retirement can come with many sudden and dramatic alterations to how we live our lives. This reality can create the potential for mental health issues to develop.
- Written by Christian Simmons
Christian Simmons
Financial Writer
Christian Simmons is a writer for RetireGuide and a member of the Association for Financial Counseling & Planning Education (AFCPE®). He covers Medicare and important retirement topics. Christian is a former winner of a Florida Society of News Editors journalism contest and has written professionally since 2016.
Read More- Edited By
Lee Williams
Lee Williams
Senior Financial Editor
Lee Williams is a professional writer, editor and content strategist with 10 years of professional experience working for global and nationally recognized brands. He has contributed to Forbes, The Huffington Post, SUCCESS Magazine, AskMen.com, Electric Literature and The Wall Street Journal. His career also includes ghostwriting for Fortune 500 CEOs and published authors.
Read More- Published: December 14, 2021
- Updated: May 23, 2023
- This page features 16 Cited Research Articles
Featured Experts
Daniel Jimenez, Associate Professor of Psychiatry and Behavioral Sciences at the University of MiamiDr. David Steffens, Professor and Chair of Psychiatry at the University of Connecticut Health CenterEmily Allen, Senior Vice President of AARP Foundation ProgramsEric Loucks, Director of the Mindfulness Center at Brown UniversityRead their full bios below the article. - Edited By
Twenty percent of adults 55 or older deal with some kind of mental health issue, according to the Centers for Disease Control and Prevention.
Americans nearing retirement are especially at risk of developing mental health issues. Older people often deal with new or reoccurring health problems, the loss of friends or loved ones and a sense of life slowing down. It’s a lot for anyone to handle.
“You have the convergence of these issues where it may not be one thing that sets you back but the culmination of things that really has an impact on health and wellbeing,” AARP Foundation Programs Senior Vice President Emily Allen told RetireGuide.

— Emily Allen, Senior Vice President, AARP Foundation Programs
According to Dr. David Steffens, chair of UConn Psychiatry and an expert in late-life depression and dementia, common mental health issues older people and recent retirees face are anxiety and depression. These issues can range from mild to debilitating and can have a major impact on how retirees live.

Common Causes of Depression in the Elderly
According to the National Institute on Aging, depression in older adults can be brought on by a major life event or change — like retirement — or significant amounts of stress. Depression can also manifest for no clear reason at all.
Several common factors occur around retirement age that can potentially cause depression and anxiety in seniors, according to Steffens.
- Prior history with depression and anxiety
- Leaving a career
- Losing loved ones
- Declining physical health
Prior History
The National Institute on Aging has found that older people who had depression when they were younger can be more likely to develop those issues again later in life.
“One risk for depression and anxiety in older adults is prior history of that,” Steffens told RetireGuide. “Any kind of major life change or stress can bring that about.”
Though older people who are facing mental health issues again may have strategies or a support system in place, Steffens recommends that those at risk of depression and anxiety always seek help from a therapist or primary care physician.
Leaving Your Career Behind
According to the U.S. Census Bureau, one in every five Americans will be at retirement age by 2030, which would create a demographic shift where older people will outnumber children for the first time in American history.
Most retirees expect to stop working full-time to enjoy a slower pace of life, pursue new activities and reconnect with their families and communities.
But Daniel Jimenez, an associate professor of psychiatry and behavioral sciences at the University of Miami, has found that it’s not nearly that simple.
“Retirement plays a huge role in mental illness because when somebody asks you ‘tell me about yourself,’ what’s the first thing you say? You mention what you do. And when you retire, you’re no longer that. So, there’s a certain loss of identity,” Jimenez said.

— Daniel Jimenez, Associate Professor of Psychiatry and Behavioral Sciences, University of Miami
Jimenez, an expert in cognitive behavioral therapy in older adults, told RetireGuide that jobs and careers for working professionals serve as more than a way to earn money — they provide structure to everyday life and a sense of purpose.
“When we’re left without that, we’re sort of drifting through life,” said Jimenez, who holds a doctorate in clinical psychology. “There’s a certain ‘what am I going to do now? I’m useless.’ There’s a lot of existential stuff that comes up.”
- Daily structure
- A part of your identity and purpose
- Long-term goals and commitments
- Social interaction
*Ad: Clicking will take you to our partner Annuity.org.
Losing Loved Ones
Another unfortunate reality of growing older is losing friends, family or a spouse as they age as well.
These challenging circumstances are difficult to navigate at any point in life but may be exacerbated to a greater extent with older people due to the changes that come with retirement.
“Not only having to deal with that, the loss of someone very close to you, but then also having to then reconcile with your own mortality because your time is coming soon,” Jimenez said. “We don’t know when but when you’re older, you’ve lived a lot more life than you have left.”
Declining Physical Health
Depression, while treatable, is not a normal part of aging; however, older adults are more at risk for increasing health problems, which can make them more vulnerable to mental health issues.
According to a 2021 report by the National Institute of Mental Health (NIMH), a chronic illness like diabetes or cancer can make you more likely to have mental health issues.
Similar to the NIMH report, the CDC found that the number of older adults who experience depression jumps from one to five percent in a typical population to 13.5 percent in seniors who require home health care.
- Alzheimer’s disease
- Autoimmune disorders
- Cancer
- Diabetes
- Heart disease
- Multiple sclerosis
- Parkinson’s disease
- Stroke
Along with chronic health issues, physical changes like declining eyesight and hearing can also have a negative impact on the mental health of older Americans.
“Every road leads either to or from mental illness,” Jimenez said. “Let’s say you’re having vision loss or you’re having hearing loss, which is common in older adulthood. That’s going to affect your mental health. You’re no longer able to see and our world is so dependent on vision and it’s a really big deal.”

Signs and Symptoms of Depression in the Elderly
According to the National Institute on Aging, many retirees are happy with their lives in spite of the many added challenges that come with age.
“Overall, older adults as a whole have a fair amount of resilience,” Steffens said. “They basically bring whatever toolkit that they have developed through life in terms of life stressors when they were younger, stressors within the family, stressors within work and all of that and are able to actually navigate that post-retirement period.”
But while most seniors are happy, many do struggle. Steffens said that it’s natural for older adults to have days when they don’t feel their best. But it’s important to note if bad days become a trend or if seniors experience a loss of interest in activities that they like doing. Other signs can include food not tasting as good as it used to, loss of concentration or trouble sleeping.
Eventually, this can culminate in seniors beginning to pull back and withdraw from others and parts of their life.
Depression may also manifest itself differently in older adults compared to younger generations, Steffens said.
| Warning Signs in Older Adults | Warning Signs in Younger People |
|---|---|
| Loss of interest in activities | Constant sadness |
| Trouble focusing or concentrating | A feeling of loss without having lost anyone |
| Withdrawing from life | Extremely low self-esteem |
| Trouble sleeping | Trouble sleeping |
| Loss of appetite | Loss of appetite |
Many older adults also experience anxiety, which is different from depression. According to the National Institute of Mental Health, anxiety involves anxious thoughts that don’t go away and worsen to the point that they interfere with your daily life.
Retirees are susceptible to anxiety due to the many added stressors that come with older age, from money issues to health.
“For anxiety, a lot of worrying,” Steffens said. “Thinking too much about things that you might have done, things that you might have said, things that you wish you would’ve done or said. The kind of thoughts you can’t get out of your mind.”
- Feeling irritable
- Feeling restless
- Struggling to control worries
- Struggling to concentrate
- Difficulty sleeping
Steffens also advises family members or caregivers who suspect their loved one is struggling with mental health issues to be observant of sudden changes in behavior. Negative reactions could be a sign that something else is going on.
The Role of Dementia
Dementia, a condition characterized by the impairment of brain functions, is more prevalent in older adults and can also lead to depression and anxiety.
The most common type of dementia is Alzheimer’s disease, according to the CDC.
“Usually, memory gets hit first. Everybody has the experience of going into a room and saying ‘why was I here, where did I put my keys,’ that kind of thing,” Steffens said. “But if it looks like somebody’s coming in and asking the same set of questions that they asked 10 or 15 minutes ago or an hour ago, and it really looks like the answer didn’t stick with them, that can be a sign of early memory problems.”
Unfortunately, dementia can be worsened by mental health issues — and vice versa. Older adults can experience intense stress from the symptoms of dementia as they come to terms with its effects.
Steffens also added that it is sometimes tough at first to determine if someone is dealing with depression or dementia. In these instances, doctors can provide depression treatment and then analyze how much the patient has improved.
Dementia can also lead to mental health issues in the patient’s spouse or caregiver. If your loved one has Alzheimer’s or a similar disease or condition, it’s important for you to remember to practice self-care and ask for help, if necessary.
“It’s an enormous, enormous stressor that affects the caregiver,” Jimenez said.
- Use breathing techniques.
- Try meditation or yoga.
- Eat healthy food.
- Get good sleep.
- Stay socially connected.
The Impact of COVID-19 on Elderly Depression
COVID-19 has had a profound impact on mental health that will be felt for years to come. According to the Kaiser Family Foundation, 40 percent of U.S. adults reported symptoms of anxiety or a depressive disorder during the pandemic.
In addition, anyone who decided to quarantine during the pandemic may have experienced more social isolation than normal — which was already a major issue for seniors and retirees even before COVID-19.

“The pandemic really exacerbated what was already happening there,” Jimenez said. “It gets harder and harder to interact with the outside world.”
While COVID-19 has negatively impacted mental health on a large scale, it has also increased public awareness of the social isolation and limited contact issues that some older adults regularly experience.
“If there’s a silver lining of the pandemic, it certainly is that people understand much more the impact of social isolation,” Allen said.

— Emily Allen, Senior Vice President, AARP Foundation Programs
There are now more options and pathways available to avoid social isolation and loneliness, such as Zoom, remote work and other live-streaming services.
These tools can offer retirees the opportunity to stay involved with others to alleviate potential anxiety and depression triggers without leaving their homes. It’s a long-term gamechanger for older Americans who deal with chronic health issues and may not be mobile.
“One of the things that we’re finding in the pandemic is that older adults actually are pretty good at learning how to access groups, access the internet,” Steffens said. “A lot of times it can actually be very helpful.”
Everything from religious services to support groups are now often available online with relatively ease of participation. For seniors who aren’t very comfortable navigating the internet, Steffens suggests asking younger family members to help with the setup of these tools.
Steffens and Allen pointed out several societal shifts that may benefit seniors in the long term.
- Society has a greater awareness of social isolation in retirees and older adults.
- Community-oriented events and activities like religious services and social gatherings are now available remotely.
- Older adults with chronic conditions can stay connected and social from their homes.
Treating Depression in the Elderly
Mental health is as important as physical health, but there is still a stigma surrounding the topic of mental illness in many communities. If you think that you or a loved one is dealing with some form of mental illness, the most important thing to remember is that it’s OK to get help.
“We talk about everything else but mental illness,” Jimenez said. “We talk about hearing loss, and we talk about vision loss — and these are all things that are really important — but when we’re talking about mental illness, it affects one in five … which is astronomical.”

— Daniel Jimenez, Associate Professor of Psychiatry and Behavioral Sciences, University of Miami
The steps you should take if you are struggling with your mental health depend on the resources available to you. According to Jimenez, the most ideal outcome would be for you to schedule appointments with a psychologist and psychiatrist at the same time.
You can also go talk to your primary care physician about your concerns; treat this like you would any medical issue.
“Most primary care doctors, they’ve had good training in the assessment and treatment of depression,” Steffens said.
- Schedule an appointment with your primary care physician.
- Ask for a referral to a psychiatrist.
- Schedule appointments directly with a psychologist and psychiatrist if possible.
If you are a family member or caregiver and you think your loved one has depression or another condition, it is critical that you help them to help themselves. Be ready to combat the stigma that still surrounds mental health in many older adults.
“The older generation, while they may see what’s happening with their grandchildren, they may not be willing or able to recognize what is going on within themselves and within their peers,” Jimenez said. “There still remains a very large stigma around that.”
- Note any changes in mood or behavior.
- Ask them if anything is wrong.
- Acknowledge their retirement difficulties.
- Encourage them to talk to a doctor.
- Schedule an appointment for them.
- Go with them to the appointment.
Mental Health Services for the Elderly
Older adults who are struggling should try to prioritize mental health where they can.
If you have Original Medicare, there are many mental health services and treatments that are available to you.
Medicare Part A will help handle the costs of mental health services that you receive in a hospital, like treatment or therapy.
Part B covers wellness visits, depression screenings, a psychiatric evaluation and some therapies and counseling.
Part D prescription drug plans typically are required to cover all antidepressant medications.
There are also options available to you if you have Medicaid, which is the largest payer for mental health services in the United States, according to the U.S. Centers for Medicare & Medicaid Services.
As far as online resources, MentalHealth.gov includes lots of useful information on various mental health topics, including how to identify and get help for mental illness.
- 988 Suicide & Crisis Lifeline
- The Lifeline provides 24/7 free and confidential support as well as prevention and crisis resources.
988
www.suicidepreventionlifeline.org - Mental Health America
- Mental Health America provides online tools and hosts events to help people better understand prevention, early identification and intervention.
800-969-6642
www.mhanational.org - National Alliance on Mental Illness
- The National Alliance on Mental Illness offers mental health education, support groups and a helpline.
800-950-6264
www.nami.org - Depression and Bipolar Support Alliance
- DBSA coordinates more than 600 local support groups across America and provides online 24/7 help, and audio and video casts.
800-826-3632
www.dbsalliance.org - National Institute of Mental Health
- As the lead federal agency for research on mental disorders, the NIMH offers basic information about clinical trials as well as resources for mental illness help.
866-615-6464
www.nimh.nih.gov

Finding Happiness in Retirement
For the many retirees who deal with mental health issues, there are multitudes more who are enjoying life.
According to a survey by TransAmerica Centers for Retirement Studies, 91 percent of retirees consider themselves generally happy people. And 40 percent of respondents indicated that their enjoyment of life has increased in their retired lives more than earlier years.
But there are still areas of concern that could lead to mental health struggles. The same survey revealed that 28 percent of retirees find that everyday activities are becoming difficult, and 20 percent often feel anxious and depressed.
Yet retirement can become less difficult if retirees prioritize creating structure in their day-to-day lives and work at staying social.
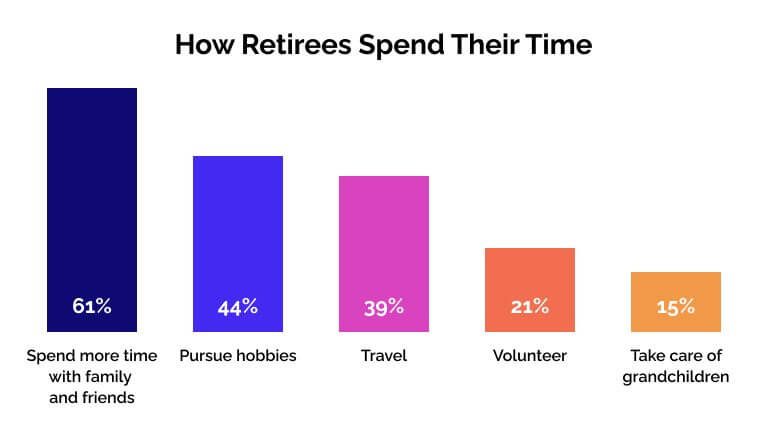
Add Structure
Having structure to each day is an absolute must, especially in retirement when seniors have more time on their hands.
If you’re physically able, one option to consider is to find a part-time job or to do volunteer work.
According to U.S. News & World Report, finding a job in retirement can provide a better life balance, offer social interaction and give you more money for a better lifestyle. Is there an industry you always wanted to work in but never did? Find something that is meaningful to you and can provide a few hours to structure your week around.
“The one thing that people may want to think about in terms of structuring their time is opportunities to go back as what they call ‘retired re-hirees,’” Steffens said. “Doing part-time work so that there is still some structure built in and it’s not just day-in day-out where your time is on your own and you don’t know what to do with it.”
Workforce changes brought about by the pandemic have also created a variety of opportunities for the chronically ill or those who can’t easily find work.
Stay Social
There are few quicker routes to mental health issues than social isolation and loneliness. According to AARP, people who live in isolation end up living shorter and less happy lives.
Isolation is a problem that older adults have faced for years — making it critical for them to find ways to stay connected to family members and friends.
“We really encourage people to make a social connection plan as they age,” Allen said. “When we think about being kids, we’re in school, we’re making friends, we’re going in groups. But often, we may as older adults think about a financial plan or a housing plan or something like that, but we don’t always think about a social connection plan.”
Allen touched on some of the considerations that go into developing a sound social connection plan.
- Identify where you will live. Are you switching communities?
- Figure out how to stay connected in your community through clubs, groups or other options.
- Talk with family and friends about staying connected. Make the effort.
- Account for changes over time, like reduced driving or less mobility.
For older adults, it’s become easier to stay connected or make new friends with other retirees through online clubs and activities over social networking applications.
Or they can opt for in-person options, such as inviting friends over to their homes, picking up part-time jobs or volunteering their time.
Practice Mindfulness
Though it’s not an alternative to medical treatment, mindfulness has emerged as an increasingly popular way to calm the mind by tracing thoughts and emotions.
Eric Loucks, director of the Mindfulness Center at Brown University, explains mindfulness and how it can benefit older adults who live with depression.

Eric Loucks has had a personal mindfulness meditation practice for almost 20 years. His work has appeared in TIME Magazine, U.S. News & World Report, CNBC and The Washington Post.
- What is mindfulness?
It’s present moment awareness of our thoughts and emotions and physical sensations. But in a nonjudgmental way, with curiosity and acceptance, gentleness.
Another piece of mindfulness that scholars have been emphasizing more lately that is in a lot of the original translations is an element of remembering. One of the best explanations I’ve seen is it’s like remembering our wisdom in this moment and applying it in this moment. Especially for people who are retired, they have decades and decades of wisdom. Part of mindfulness is bringing that wisdom to this very moment and applying it.
- What are the benefits of practicing mindfulness?
The evidence of the impacts of mindfulness on loneliness are quite strong. I practice in a meditation group that has a lot of retired older individuals and a lot of them are living on their own. Part of what mindfulness does is it creates the present moment to be a fuller experience. Even if you’re not with someone in that moment and savor just doing dishes. Can we just be there with the dishes and then notice where the mind goes?
Does it go to the past? Does it go to the future? Does it usually go to the past? Does it usually go to the future? In those moments, not only are we practicing our cognitive skills and our ability to be right here for our life as it is right now, but we are also learning about ourselves and growing in the process.
Whether we’re with someone or not, feelings of loneliness can actually go down because those moments alone can be more meaningful. But also a lot of people practice mindfulness in groups, and that can create new opportunities for friendship. In my mindfulness training, most people are retired and they’re joining by Zoom. We hear about each other’s lives every week and get updates and then support each other.
- How can this benefit older adults who live with depression?
One of the ways that it seems to help is helping us avoid what they call repetitive negative thinking, or rumination. When we’re experiencing depression, we can get into these downward negative thought spirals where one negative thought can lead to another one, and we can have a tough time breaking out of that.
What mindfulness training does is it trains us to become more aware of our emotions and more aware of our thoughts. More aware of our body, where we’re feeling the tension in our body related to depression. And so, we become better at knowing when we’re having a negative thought pattern.
- Is it difficult to start practicing mindfulness?
I think of meditation as a slow fix rather than a quick fix. It’s kind of like going to the gym for our muscles. For my first 15 years or so meditating, I meditated 10 to 20 minutes a day, so it wasn’t a huge amount. And I got a lot of benefits just out of those 10 to 20 minutes.
It can be certainly challenging for some but just like anything, it does take energy. It takes energy to eat healthily, to learn how to select the foods and to cook them and to eat whole foods. It takes energy to get physical activity. But those are some of the biggest things we can do that can help us be successful at healthy aging.
- How can someone get started?
There’s lots of entry points. There’s lots of really good books on mindfulness, and you can just pick up a book on it. There are some apps like Headspace or Calm. If you’d like to have a live teacher online, the Mindfulness Center at Brown that I’m the director of, we have free daily programs so they can just go to brown.edu/public-health/mindfulness/ and you can log in anywhere in the country, anywhere in the world to our teacher-led mindfulness program. That gives you a teacher, gives you some teachings and it also gives you a community of other people that are practicing.
Google mindfulness and meditation in the city or town that you live in and just see what comes up because it’s getting so popular now that you might well find a community that’s a good fit for you.
It may sound almost too simple but it’s also true: So much of happiness and health in retirement is having a structure to your life and having friends to join you on your path. If you don’t have those things yet, there are many ways to get them. And above all, it’s important to ask for help.
“For a whole host of reasons — stigma, lack of understanding, a whole bunch of stuff — we don’t want to talk about [mental health],” Jimenez said. “But it’s something that needs to be dealt with.”
16 Cited Research Articles
- National Institute on Aging. (2021, July 7). Depression and Older Adults. Retrieved from https://www.nia.nih.gov/health/depression-and-older-adults
- Kaiser Family Foundation. (2021, February 10). The Implications of COVID-19 for Mental Health and Substance Use. Retrieved from https://www.kff.org/coronavirus-covid-19/issue-brief/the-implications-of-covid-19-for-mental-health-and-substance-use/
- National Institute of Mental Health (2021). Chronic Illness and Mental Health: Recognizing and Treating Depression. Retrieved form https://www.nimh.nih.gov/health/publications/chronic-illness-mental-health
- AARP. (2020, December 29). 5 Secrets to a Happy Retirement. Retrieved from https://www.aarp.org/retirement/planning-for-retirement/info-2020/5-secrets-to-retire-happy.html
- Sightings, T. (2019, May 22). The Pros and Cons of Working in Retirement. Retrieved from https://money.usnews.com/money/retirement/second-careers/articles/inflation-and-retirees-when-to-think-about-going-back-to-work
- Centers for Disease Control and Prevention. (2019, April 5). What is Dementia? Retrieved from https://www.cdc.gov/aging/dementia/index.html
- TransAmerica Center for Retirement Studies. (2018, December). A Precarious Existence: How Today’s Retirees are Financially Fairing in Retirement. Retrieved from https://transamericacenter.org/docs/default-source/retirees-survey/tcrs2018_sr_retirees_survey_financially_faring.pdf
- Myers, K. (2018, November 21). Americans are retiring at an increasing pace. Retrieved from https://www.yahoo.com/now/americans-retiring-increasing-pace-145837368.html
- National Institute of Mental Health (2018, July). Anxiety Disorders. Retrieved from https://www.nimh.nih.gov/health/topics/anxiety-disorders
- National Institute of Mental Health (2018, March). Older Adults and Mental Health. Retrieved from https://www.nimh.nih.gov/health/topics/older-adults-and-mental-health
- National Institute of Mental Health (2018, February). Depression. Retrieved from https://www.nimh.nih.gov/health/topics/depression
- AARP (n.d.). Connect Tools to Overcome Social Isolation. Retrieved from https://connect2affect.org/
- American Foundation for Suicide Depression. (n.d.). Suicide prevention resources. Retrieved from https://afsp.org/suicide-prevention-resources
- Brown School of Mental Health (n.d.). Mindfulness Center at Brown. Retrieved from https://www.brown.edu/public-health/mindfulness/
- Centers for Disease Control and Prevention. (n.d.). The State of Mental Health and Aging in America. Retrieved from https://www.cdc.gov/aging/pdf/mental_health.pdf
- U.S. Centers for Medicare & Medicaid Services. (n.d.) Behavioral Health Services. Retrieved from https://www.medicaid.gov/medicaid/benefits/behavioral-health-services/index.html
Calling this number connects you to one of our trusted partners.
If you're interested in help navigating your options, a representative will provide you with a free, no-obligation consultation.
Our partners are committed to excellent customer service. They can match you with a qualified professional for your unique objectives.
We/Our Partners do not offer every plan available in your area. Any information provided is limited to those plans offered in your area. Please contact Medicare.gov or 1-800-MEDICARE to get information on all of your options.
844-359-1705Your web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you need help pricing and building your medicare plan, call us at 844-572-0696





