What Seniors Can Expect As the COVID-19 Vaccine Becomes Available
- Written by Rachel Christian
Rachel Christian
Financial Writer and Certified Educator in Personal Finance
Rachel Christian is a writer and researcher for RetireGuide. She covers annuities, Medicare, life insurance and other important retirement topics. Rachel is a member of the Association for Financial Counseling & Planning Education.
Read More- Published: December 15, 2020
- 5 min read time
- This page features 18 Cited Research Articles
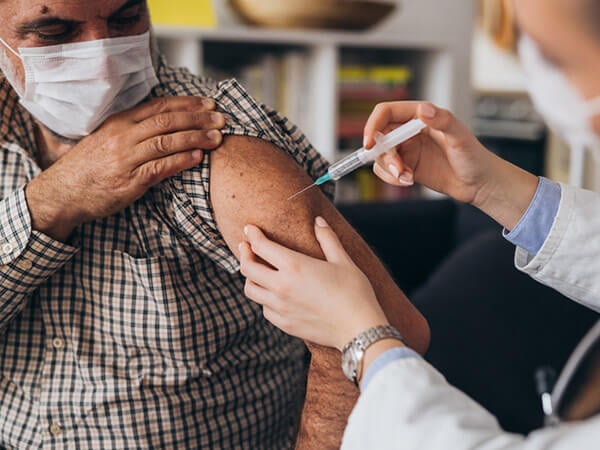
Residents at long-term care facilities are set to become some of the first recipients of a new COVID-19 vaccine.
The Food and Drug Administration issued an emergency use authorization for the Pfizer-BioNTech COVID-19 vaccine on Dec. 11. The authorization allows the vaccine to be distributed in the U.S.
After long-term care residents and health care workers, other seniors ages 65 and older may receive vaccine priority, although many unknowns remain.
Medicare — the largest health care provider for older Americans — has already enacted new rules that allow beneficiaries to receive the COVID-19 vaccine for free once it becomes available.
CDC Advisory Committee Green Lights Long-Term Care Residents for First Round of Vaccinations
On Dec. 1, the Advisory Committee on Immunization Practices — an expert panel that advises the Centers for Disease Control and Prevention — voted to recommend giving residents at long-term care facilities high-priority access to the COVID-19 vaccine during the first rollout.
Roughly 3 million Americans reside in nursing homes, assisted living facilities and other group-care communities, according to the CDC.
Dr. Moncef Slaoui, chief science adviser of Operation Warp Speed — the Trump administration’s program to rapidly develop and distribute vaccines — said that residents of long-term care facilities will receive the first round of vaccinations by mid-January, according to The New York Times.
“Based on the data we’ve seen so far, rushing the vaccine to nursing homes should reduce the number of deaths that would otherwise occur due to COVID,” Tricia Neuman, executive director of the Kaiser Family Foundation’s Program on Medicare Policy and senior advisor to the president, told RetireGuide.
The federal government has contracted with national pharmacy chains CVS and Walgreens to distribute the vaccine with no out-of-pocket costs, according to the U.S. Department of Health and Human Services.
CVS and Walgreens will schedule and coordinate directly with each long-term care facility to establish on-site clinics.
HHS anticipates that three visits over about two months will be needed to administer both doses of the vaccine.
“Our unprecedented public-private partnership with CVS and Walgreens will provide convenient and free vaccination to residents of nursing homes across America,” HHS Secretary Alex Azar stated in an October news release.
This frail and elderly population has suffered the greatest coronavirus-related casualties in the U.S.
COVID-19 has killed more than 100,000 long-term care facility residents and staff as of Nov. 24, according to an analysis of state-reported data by the Kaiser Family Foundation.
Older adults in general are at greater risk of requiring hospitalization or dying if diagnosed with COVID-19, according to the CDC.
If initial vaccines are in short supply, skilled nursing facilities should be prioritized among other types of long-term care venues because they house the most medically vulnerable residents, according to the CDC.
State officials will ultimately be responsible for making their own distribution plans. Strategies vary considerably among states, according to AARP, USA Today and other news sources.
Vaccines are being studied in older adults with underlying health conditions in clinical trials. However, long-term care facility residents have not been specifically studied.
Medicare Rules to Make Vaccine Free to All Beneficiaries
On Oct. 28, the Centers for Medicare & Medicaid Services, or CMS, released an Interim Final Rule with Comment Period stating that Medicare and other programs will cover the cost of any COVID-19 vaccine authorized by the FDA.
The regulation clearly notes that any Medicare copays, deductibles or coinsurance associated with the vaccine will be waived — whether a beneficiary is enrolled in Original Medicare or a Medicare Advantage plan.
Medicare has also ruled to provide free COVID-19 testing and certain services during the public health emergency.
Free COVID-19-related services offered by Medicare include:
- Lab tests for COVID-19.
- FDA-authorized COVID-19 antibody test.
- Monoclonal antibody infusions used to treat COVID-19.
- The COVID-19 vaccine.
Medicare has also temporarily expanded its coverage of telehealth services in response to the pandemic.
This allows Original Medicare beneficiaries to receive telehealth evaluations, common office visits, mental health counseling and preventive health services virtually without a copayment.
“There’s a ton of research that shows how costs can be a barrier to care and treatment,” Neuman said. “Eliminating this barrier helps clear the path, which is particularly important for lower income people of all ages.”
It’s Unknown How Long Other Seniors Will Wait for the Vaccine
It is unclear how long Americans ages 65 and older who live outside long-term care facilities may wait to receive a vaccination. Individual states will make the final call.
The Advisory Committee on Immunization Practices — the same expert group that recommended health care workers and long-term care residents get top priority — will soon vote on who should receive the next wave of vaccinations.
In a November meeting, all voting members of the committee indicated support for putting essential workers ahead of people ages 65 and older.
But a final decision isn’t expected until later this month.
Dr. Robert Redfield, director of the CDC and the country’s top public health official, said in a statement on Dec. 3 that he “looks forward to future recommendations that, based on vaccine availability, demonstrate that we as a nation also prioritize the elderly” especially those who live in multi-generation households.
Once the ACIP votes, Dr. Redfield will decide whether to accept its recommendations as official CDC guidance.
Still, the ultimate decision on who gets the second round of vaccines lies with governors and state and local health officials.
While states have historically followed CDC guidelines, they are not required to do so.
According to The New York Times, many states plan to put at least some older people outside long-term care facilities ahead of most essential workers — but that could change after the ACIP makes its formal recommendation.