Are Insulin Prices Actually Getting Cheaper with Medicare?
- Written by Rachel Christian
Rachel Christian
Financial Writer and Certified Educator in Personal Finance
Rachel Christian is a writer and researcher for RetireGuide. She covers annuities, Medicare, life insurance and other important retirement topics. Rachel is a member of the Association for Financial Counseling & Planning Education.
Read More- Published: November 9, 2020
- 6 min read time
- This page features 12 Cited Research Articles
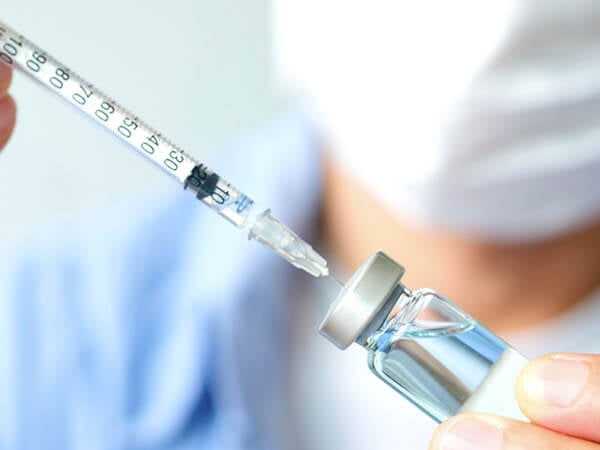
Over 34 million Americans have diabetes. Of those, 7 million require some form of insulin — including more than 3.3 million seniors on Medicare.
Insulin is a lifesaving drug that’s been around for nearly 100 years. Yet costs for the medication keep skyrocketing.
According to researchers at the Yale School of Medicine, the price of insulin has tripled in the U.S. over the last 10 years — and the out-of-pocket cost for patients has doubled.
An initiative announced by the Trump administration in March 2020 aims to lower insulin costs for seniors by capping monthly copayments at $35. Legislative efforts by Congress are also taking place.
But how effective will these measures be in making the drug more affordable — especially for older Americans?
The Cost of Insulin
The price of insulin for consumers varies widely. A patient’s out-of-pocket cost depends on several factors, including their insurance — or lack of it — the type of plan they have and discounts from manufacturers.
The amount of insulin a patient needs and the type that works best for their condition also play a role.
For example, vials of insulin cost less than insulin pens, while the price of analog insulin — or human insulin that has been genetically altered — is much more expensive than traditional insulin.
Still, on average, Type 1 diabetics paid $5,705 per-person for insulin in 2016 — nearly double what they paid in 2012, according to the Health Care Cost Institute.
“It’s important to make insulin affordable for a number of reasons, including the fact that insulin prices have risen exponentially and are unaffordable for many users,” Laura Friedman, vice president of the American Diabetes Association’s Federal Payment Policy, told RetireGuide.
Friedman said one issue with rising prices is a lack of transparency through the insulin supply chain.
The supply chain is made up of two main pathways: the delivery of insulin from manufacturers to patients and the flow of payments for insulin throughout the supply and delivery chain.
Wholesalers, pharmacists, providers, insurers and pharmacy benefit managers serve as intermediaries.
But deconstructing that complicated web is difficult — for both advocates and lawmakers alike.
“It is unclear precisely how the dollars flow and how much each intermediary profits,” Friedman said.
The American Diabetes Association’s Insulin Access and Affordability Working Group has testified before Congress and lobbied both state and federal government to take action on issues.
Medicare Coverage of Insulin and Diabetes Supplies
One-third of Medicare beneficiaries had diabetes in 2017, up from 18 percent in 2000.
Original Medicare (Part A and Part B) does not cover insulin, or other diabetes supplies such as insulin pens, syringes, needles and alcohol swabs.
Medicare Part B covers only a narrow scope of diabetes supplies, including:
- Insulin pumps
- Blood sugar monitors
- Test strips
- Lancet devices
- Lancets
For insulin and other diabetes medications, patients must enroll in a standalone Medicare Part D plan or a Medicare Advantage plan with prescription drug coverage.
These plans are administered by private insurance companies that contract with the Centers for Medicare & Medicaid Services, or CMS.
Each plan carries its own deductibles and copays. Coverage can vary widely.
For people without Part D low-income subsidies, the average annual out-of-pocket spending on insulin increased by 79 percent from 2007 to 2017, according to research by the Kaiser Family Foundation, or KFF, a nonprofit group focused on health care policy issues.
Trump’s Plan to Cap Insulin Costs
In March 2020, the Trump administration announced plans for a Seniors Saving Model to address out-of-pocket insulin costs.
The new model allows participating Part D plans to offer coverage of insulin for a monthly copayment of no more than $35.
Beneficiaries can enroll in these plans now. Changes go into effect Jan. 1, 2021.
The Part D Senior Savings Model is voluntary, which means not all drug plans will participate.
Plans participating in the new insulin model are considered “enhanced” plans, which offer a wider range of benefits but also feature pricier premiums.
In 2020, the average monthly premium for enhanced Part D plans was $47 compared to $30 for basic plans, according to KFF.
CMS estimated that the model will increase enhanced plan premiums by an additional $1 per month.
However, enhanced plans can offer lower deductibles and higher initial coverage limits compared to basic Part D plans.
The new model does not address affordability issues for the uninsured or people covered by other health care insurance besides Medicare.
Limited Time to Switch to a New Plan
A total of 1,635 enhanced Part D plans are participating in the Senior Savings Model nationwide for calendar year 2021, according to CMS. For context, that’s about half of all enhanced Medicare Advantage and standalone Part D plans in 2020.
KFF estimates that one-fifth of Part D users may need to switch from a basic plan to an enhanced plan to receive these lower-cost insulin benefits.
Some additional beneficiaries who are already enrolled in an enhanced plan will also need to switch if their current plan has chosen not to participate in the Senior Savings Model.
Medicare users are under a time crunch to explore their options.
Generally, you can only switch to a different Part D or Medicare Advantage plan during the annual open enrollment period, which is going on now through Dec. 7.
People who are already enrolled in a Medicare Advantage plan and want to switch to a different one also have an opportunity to do so from Jan. 1 to March 31.
Beneficiaries can use the online Medicare Plan Finder to compare options.
CMS has added a filter to make it easier for users to identify plans with capped out-of-pocket costs for insulin in the model.
Insulin Pump Users are Unaffected by Trump’s New Model
Not all seniors who take insulin will benefit from the new cap model, including patients who use insulin pumps instead of injectable insulin.
Insulin used in pumps is covered by Medicare Part B, not Part D, and therefore isn’t affected by the new model.
An August 2020 analysis reports that insulin pump users spend an average copay of $54.26 a month — over 50 percent more than the Senior Savings Model cap.
From December 2016 to June 2018, the cost of pump-delivered insulin increased 304 percent, according to the analysis.
Legislative Proposals Also Aim to Lower Insulin Cost
Several bills that aim to curb insulin costs for consumers have been introduced in the current Congressional session.
Current Bills in the 116th Congress That Address Insulin Prices
- Lower Costs, More Cures Act: A sweeping House health care reform bill introduced by Republicans that includes a provision to place an out-of-pocket cap of $50 on insulin and insulin medical supplies for Medicare beneficiaries.
- Insulin Access for All Act: A House bill introduced by Democrats that proposes eliminating deductibles, copayments and coinsurance for insulin and any medical supplies needed to inject insulin for Medicare and Medicaid beneficiaries.
- Affordable Insulin Act: A House bill introduced by Democrats that would allow the importation of affordable and safe insulin by wholesale distributors, pharmacies and individuals from Canada and other qualifying countries.
- End Price Gouging for Insulin Act: A House bill introduced by Democrats that would require the Secretary of Health and Human Services to establish an annual reference price for insulin products sold under any federal health program, including Medicare, based on existing prices in similar countries; it would also impose penalties on manufacturers that do not comply with these prices.
- Insulin Price Reduction Act: A bipartisan House bill that would prohibit manufacturer rebates for insulin products, which often act as an incentive to raise list prices; it would make the price an insurer pays for a drug closer to what an uninsured individual might pay for the drug.
Most of these proposals passed the House but stalled in the Senate. The current Congressional session ends in January 2021.
Calling this number connects you to one of our trusted partners.
If you're interested in help navigating your options, a representative will provide you with a free, no-obligation consultation.
Our partners are committed to excellent customer service. They can match you with a qualified professional for your unique objectives.
We/Our Partners do not offer every plan available in your area. Any information provided is limited to those plans offered in your area. Please contact Medicare.gov or 1-800-MEDICARE to get information on all of your options.
866-749-5443